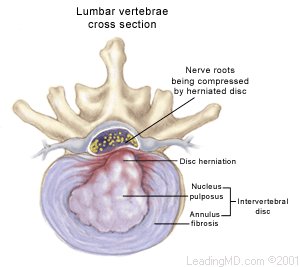
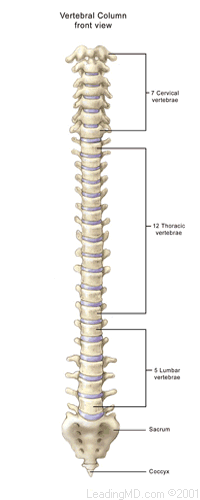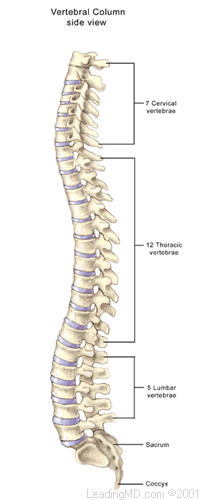
How is a herniated lumbar disc treated?
Non-operative treatment for the first 4-6 weeks:
Except in a few special circumstances, initial treatment for herniated discs should be conservative. People with back pain and sciatica are treated alike, with emphasis on pain relief and early mobilization. Fortunately, herniated discs improve without surgery about 80% of the time. It usually takes four to six weeks of conservative treatment before a patient can resume normal activities. One research study investigated the results of conservative versus operative treatment for herniated discs. It showed that surgical patients did better when checked at 1, 2 and 4 years. After ten years, however, the two groups were doing equally well, indicating that eventually the pain associated with herniated discs resolves on its own.
-
Narcotic pain medicines: If the first few days are extremely painful, narcotic pain medicines are often prescribed. Some of these are safe for short periods, but have worrisome side effects when used for a long period of time.
-
Anti-inflammatory medicines: Since inflammation of the spinal nerves and back muscles contribute to the problem, anti-inflammatory medicines are frequently prescribed. These are often called "arthritis medicines" or "NSAIDs" (non steroidal anti inflamatory drugs) It usually takes several days of treatment before NSAIDs are fully effective. Some NSAIDs may cause acid stomach so they should generally be taken with food.
-
Muscle relaxers: These medicines are given to help ease muscle spasm. Their usefulness is controversial, and they tend to make patients drowsy.
-
Oral corticosteroids: These powerful anti-inflamatories have many side effects so their use is limited. The side effects of upset stomach, mood swings and changes to the endocrine system are minimized if the length of treatment is limited to a week. These medicines are often given in tapering doses daily for 7 to 10 days and then stopped.
-
Physical therapy: Physical therapists have several treatments that can help loosen cramped muscles and ease pain. One very important contribution they make is to get the patient started on a specific exercise program to strengthen the stomach and back muscles after the initial spasms have subsided. An ongoing commitment to a home exercise program is the best way to protect against a recurrence of back problems.
Non-operative treatment after the first 4-6 weeks:
-
Most people improve steadily and gradually for several weeks, then hit a plateau. When this plateau is still unacceptably painful, the following treatments may be considered. It is important to determine whether the pain is more in the leg or more in the back.
-
Patients with leg pain predominating (sciatica) may have the diagnosis confirmed by an MRI of the lumbar spine or a myelogram/CT scan. Two non-surgical treatments that can be helpful:
-
Epidural steroid injection (ESI): The MRI may suggest that an injection of corticosteroid (sometimes known as "cortisone") directly around the spinal nerves, may be helpful. This is a special procedure. ESIs are very safe, but the decision to have one should only be made after a discussion with the physician.
-
A selective nerve root block (SNRB) is an injection which treats only one nerve. Frequently, epidurals and selective nerve root blocks are done with X-ray control to make sure the medicine is placed exactly where it is needed.
Herniated Disc Patients With Back Pain Predominating:
There are three main treatments for patients who have back pain rather than sciatica:
-
Exercise:The mainstay of treatment for back pain is a good self directed home exercise program to increase abdominal strength, back muscle strength, and flexibility. There are many theories on which exercises are best. A physical therapist trained in back care will develop a personalized program with the patient over a one to three week period. Good abdominal strength is the key to a healthy back, therefore it is important for the patient to continue these exercises indefinitely.
-
Anti-inflammatory medicines (NSAIDs):These are often called arthritis medicines. It is important for the patient to give them a full three to four week trial since it takes this length of time for them to become fully effective. There are many types, and each individual can probably find one or two that work well.
-
Bracing: If symptoms persist over a long period of time, and exercise and NSAIDs have not improved the condition, a brace may be worn to provide additional support to the painful disc. When used with a good abdominal strengthening program, a brace may allow some people to be more active with less pain. Patients should choose a brace that is comfortable enough to wear for several hours at a time for the more strenuous activities.
Operative Treatment for Patients with Leg Pain Predominating
The 20% who do not respond to treatment after at least four to six weeks of non-surgical treatment and a few who have special problems may benefit from surgery, such as a microdiscectomy: a microscopic removal of the disc rupture to decompress the pinched nerve. Click to Enlarge
The indications for surgery include:
-
Intense leg pain.
-
The MRI shows a ruptured disc compressing a nerve which is consistent with the distribution of the leg pain.
-
Testing the nerve by stretching it ("nerve root tension signal") reproduces the leg pain.
-
There are no factors that would make surgery a risk for the patient.
-
Progressive worsening of nerve function, such as any loss of bowel or bladder function.
The Surgical Procedure: Microdiscectomy
The operation usually lasts one to two hours and provides good or excellent results in 95% of cases. Leg pain does not disappear immediately after surgery, but gradually disappears over several weeks.
-
A general anesthetic is used, and once asleep,the patient is placed in the prone or kneeling position on a specially padded frame.
-
A small incision is made directly over the disc, and a microscope is then used to find the compressed nerve and move it aside so that the ruptured portion of the disc can be seen and removed. Only the ruptured portion and loose pieces within about ½ inch of the hole are removed.
-
The space around the nerve is then thoroughly examined to make sure no small pieces of disc material might still compress the nerve.
-
Finally, antibiotic solutions are washed through the disc and incision to reduce the chances of infection. An absorbable suture is used to close the incision so that there are no stitches to be removed later.
What types of complications may occur?
All surgeries have risks, but complications with this procedure are few. Nevertheless, it is important for the patient to have a thorough discussion of these and other potential risks with the doctor before making a decision to have surgery.
-
Scar tissue formation (a 5% chance):When this surgery fails, it is due to an overgrowth of scar tissue around the nerve. Most people form some scar tissue in the area of a surgery, but for unknown reasons, some individuals form an extraordinary amount of scar which surrounds and irritates the nerve. It can form along the spinal nerve inside the spinal canal, or where the nerve exits the spine.
-
Infection (a 3-5% chance): Wound infection can happen any time an incision is made. The bacteria can come from the skin around the incision, the air in the operating room, or the bacteria that circulate in the bloodstream. The steps taken in the operating room to avoid infection are many. A dose of intravenous antibiotics right before surgery reduces the risk of infection even more. Persistent drainage from the wound 4-7 days after surgery usually means an infection is present. The patient might also have fever or chills, but this is not a reliable indication of an infection. Antibiotics are usually successful, but sometimes it is necessary to return to the operating room to wash out the incision. An infection does not usually cause the operation to fail, but may slow the healing process.
-
Spinal fuid leak (approximately 1%): Spinal fluid bathes the spinal cord and is contained inside a sac called the dura mater. Sometimes scar tissue forms between this sac and the ruptured disc. A hole can develop in the dura when the surgeon is looking for or removing the ruptured disc, allowing spinal fluid to leak out. When a spinal fluid leak is encountered, the hole is immediately repaired. Sometimes artificial blood clot is added to form a seal around the repair. Usually the patient is kept flat for 24 hours to allow the hole to heal before resuming a normal recovery.
-
Nerve damage at surgery (<1% chance): A nerve that has been compressed by a ruptured disc can be very fragile. Just moving the nerve to get at the disc behind it might cause this fragile nerve to be damaged. Fortunately, this is very rare, as is other surgical damage to the nerve.
-
Bleeding (rare): Blood loss is a rare complication . People whose blood does not clot blood normally are at increased risk. The large blood vessels in front of the spine may be damaged while removing disc material from within the disc. This is extremely rare (perhaps one in ten thousand cases) and requires emergency abdominal surgery to repair the bleeding vessel.
-
Recurrence (7%): Though technically not a complication of surgery, there is about a seven percent chance that the same disc will rupture again, most likely in the first six weeks after surgery when the hole in the disc annulus is healing. Even after six weeks the disc continues to be prone to injury. This is why the maximum weight a patient should lift is 8-10 pounds for six weeks after surgery. Abdominal strengthening exercises are recommended for life, since strong stomach muscles are good insurance against recurring disc problems.