The knee is a commonly injured joint. Within recent years, the increase in ACL (anterior cruciate ligament) injuries has been remarkable. Trauma to this ligament within the knee can be serious, and injuries to it usually occur during athletic activity.
Why are knee injuries so common?
The knee is particularly vulnerable to injury. It is the joint between the two longest bones of the body, and the entire weight of the body is transferred to the foot through the knee. The knee is also more prone to injury because its stability decreases as it bends. The menisci and the ligaments provide less effective support to the bent knee.
What does the inside of the knee look like and where is the ACL?
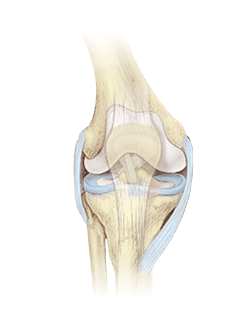
The knee joint contains bones, ligaments, muscle tendons, cartilage, nerves, and blood vessels. A fibrous joint capsule made of collagen surrounds the joint and encircles the end of each bone to give the knee stability.
Overview
What does the ACL do?
The anterior cruciate ligament is one of two ligaments inside the knee joint (the other is the PCL ). This ligament runs from the top surface of the tibia diagonally into the large notch at the end of the femur. The ACL prevents the tibia from sliding too far forward underneath the femur. It also helps prevent overstraightening and over-rotation of the femur on the tibia.
What is an ACL injury?
An ACL injury usually occurs when the knee is sharply twisted or extended beyond its normal range of motion.
The three grades of ACL injury range from mild to severe.
Grade I - Trauma to the ligament is relatively minor. Some of the fibers are stretched. This is considered a "sprain".
Grade II - Trauma to the ligament is more severe. Some of the fibers are torn. This is called a "partial tear".
Grade III - This is the most severe ACL injury. The fibers of the ligament are completely torn. It is referred to as a "complete tear".
Sports in which the foot is planted, the knee is bent, and change in direction is emphasized are commonly associated with ACL injuries. Basketball, skiing, and football are examples of sports in which a high number of ACL injuries occur. These sports require movements that cause the femur to pivot on the tibia. Skiing has additional risk factors that increase the chances of ACL injury. The length of the ski adds more force to the twisting motion. The stiffness and height of the ski boot cause the forces to be transferred up the leg to the vulnerable knee joint.
The ACL is also very susceptible to injury in contact sports. It can be damaged along with the medial collateral ligament (MCL) when the knee is struck from the outside. A hit that results in the tibia being driven forward, the femur being driven backward, or the knee joint being severely hyperextended may result in damage to the ACL.
Females appear to be more at risk for ACL injuries. Competitive female soccer and basketball players have 3-5 times higher risk of ACL injury than their male counterparts. Why do females seem more likely to injure the ACL when they play the same sports as males? Many studies are looking at the physical differences between the sexes for answers to this question.
Two differences are size and strength. The ACL and the notch (illustration) on the femur that it sits in are smaller in women than in men, but that may just be because women are smaller than men. The male's lower percentage of body fat and greater muscle mass give the male an advantage in muscular strength to protect the ACL.
Other differences make the female a more likely candidate for ACL trouble than her male counterpart. The mechanics of the woman's body, with the pelvis creating a larger angle from hip to knee, may make the knee more prone to injury. Neuromuscular differences in the timing of muscle activation and how women perform risky movements may increase the female's vulnerability to ACL injury. Women tend to change direction and land from jumps in a more erect stance, and this can put the ACL under strain. Hormonal differences focus on estrogen in the female body and its effect on ligament laxity and knee looseness. Although these theories have not been proven, agility training and muscle strengthening seem to be appropriate measures women can take to help prevent injury.
What are the signs and symptoms of an ACL injury?
A twist or strain has occurred which causes the following signs:
- "Pop" - Many patients, but not all, will hear or feel a "pop" when the ACL tears.
- Immediate onset of swelling - This is an indication that there is bleeding from the injured ligament.
- Pain - Most patients experience quite a bit of pain with an ACL injury.
- Instability - Patients often describe a buckling or unstable sensation in the knee.
How is an ACL injury diagnosed?
The orthopaedic surgeon will want to know the history of the knee injury and will determine if the signs and symptoms of an ACL injury are present.
After taking a history, the orthopaedic surgeon will perform a physical examination. The doctor will perform manual tests on the knee to determine the amount of instability that exists. The Lachman Test, Anterior Drawer Test, and Pivot Shift Test are exams the doctor may use to see how much the tibia moves in relation to the femur.
Pain, swelling, and muscle spasms in the early stages of an injury may make it difficult for the doctor to diagnose the degree of instability with manual tests. An arthrometer, a machine that measures joint looseness in the knee, may be used.
X-rays can reveal signs of bone fractures, chips, or arthritis. Since X-rays can only show bone, a Magnetic Resonance Image (MRI) may be ordered to assess damage to soft tissue such as ligaments, tendons, and cartilage. An MRI is a non-operative procedure that allows the surgeon to determine the amount of damage to the ACL and any other structures of the knee.
If further testing is needed to clearly evaluate the problem, an arthroscopy may be recommended. During an arthroscopy, a tiny fiberoptic scope is inserted into the joint. The doctor uses this scope to visually assess the damage. In most cases, a diagnosis can be made without using this surgical procedure.
How is an ACL injury treated?
The common recommendation for immediate treatment of an ACL injury is the well-known rule of RICE:
- Rest the knee by using crutches and keeping weight off of it
- Ice the knee
- Compress the knee with a wrap
- Elevate the leg
These measures will help control swelling. The doctor may also drain the joint of excess fluid to reduce pressure.After the initial injury symptoms have subsided and the diagnosis has been established, the orthopaedic surgeon will look at the history of the injury and the patient's activity level to determine what treatment is best for the patient.
- How old is the knee injury?
- Does the patient continue to have recurrent instability?
- How old is the patient and what types of activities does this patient enjoy?
- What level of activity does this patient wish to return to?
- Are there other associated injuries?
- The two basic treatment choices for an ACL injury are:
- Non-operative treatment with rehabilitation and bracing
- Surgical treatment
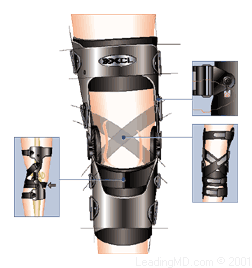 Non-operative Treatment
Non-operative Treatment
The ACL does not reliably heal well on its own. Although this is true, about one-third of all patients will do well without surgery. A patient who does well without surgery is:
- older or less active
- one who decreases his or her activity level
- one who avoids pivoting sports
These patients can expect a fair to good outcome just by learning to cope with their injury.
Patients who do not do well with non-operative treatment are usually described as:
- younger or active patients
- those who like to participate in pivoting sports
These patients are more at risk for reinjury. For these people, the likelihood of further damage to other ligaments or cartilage is quite high. A common reinjury is tearing a meniscus, which can lead to degenerative arthritis in the years to come.
Patients who are less active and do not participate in pivoting sports can continue to have a high quality of life with a good rehabilitation program. A partial tear to the ACL is usually treated in this manner.
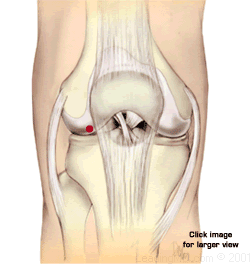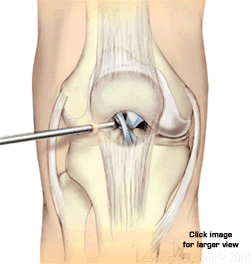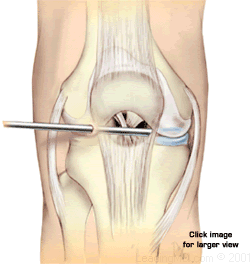 Operative Treatment
Operative Treatment
Patients for whom surgery is generally recommended:
- Active individuals who participate in any sport with pivoting - such as soccer, tennis, basketball, football, or skiing
- Patients who continue to experience instability after going through a rehabilitation program
- Those with injuries involving more than one ligament
It is important to consider the patient's commitment to the rehabilitation program following an ACL surgical procedure. This is especially critical if a meniscal repair is also required. The patient must agree to carefully follow the recovery timetable outlined by the doctor.
The timing of an operation is important to prevent stiffness after surgery and obtain the best results. It is helpful when:
- range of motion is adequate
- swelling is reduced
- quadricep muscles are functional
It often takes about three weeks for the knee to reach this point.
Is there a simple way to repair the damaged ACL without a reconstruction?
In a direct repair the ends of the torn ligament are sewn together. This procedure is usually not recommended, as the ends of the ligament do not heal reliably. Direct repairs of the ligament to the bone may heal; however, this, also is not always reliable.
Extra-articular (outside the joint) procedures involve securing a portion of a tendon on the outer part of the knee (the iliotibial band) across the outside of the joint. This procedure does not reconstruct the torn ACL. It attempts to provide increased stability by placing a restraint on the outside of the knee. This procedure is generally not adequate by itself but it is occasionally done to provide additional support after ACL reconstruction.
Replacing the damaged ACL with a graft made of synthetic materials is no longer performed due to poor results. Many patients who had this surgery experienced reactions to the synthetic material as well as early failures of the graft.
An ACL reconstruction is the most common surgical procedure performed today since it usually produces the best results.
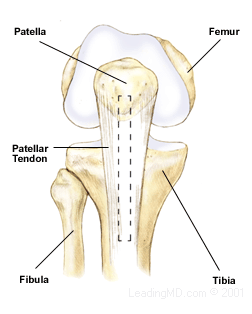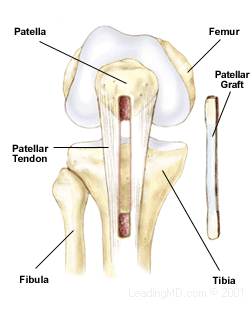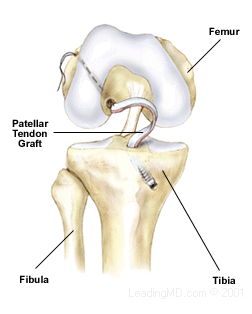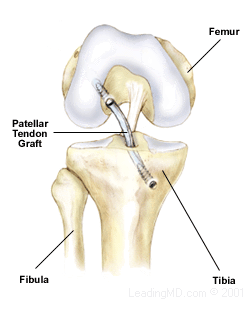 An ACL reconstruction is a surgical procedure that involves removing the remains of the damaged ACL and replacing it with another form of soft tissue, called a graft. The graft is either autogenous, which comes from the patient, or an allograft, which is tissue donated by an individual at the time of death.
An ACL reconstruction is a surgical procedure that involves removing the remains of the damaged ACL and replacing it with another form of soft tissue, called a graft. The graft is either autogenous, which comes from the patient, or an allograft, which is tissue donated by an individual at the time of death.
In both cases, a portion of the patellar tendon is commonly used to replace the ACL. This is the tendon of the quadriceps muscles that attaches the patella to the tibia. This is a popular choice among surgeons because the patellar tendon is a large, strong tendon, and bone is taken at each end with the tendon section. The bone ends are attached to the femur and tibia, allowing for bone-to-bone healing. The bone plugs fuse in place during healing and create the strongest fixation possible. This technique usually heals faster than when soft tissue is attached to bone.
Another popular graft choice incorporates strands from one of the smaller hamstring tendons (the semitendinosus) the gracilis replace the ACL. Although this graft requires soft tissue-to-bone healing, many surgeons prefer it because there is usually less pain associated with the harvesting technique of the graft. Some surgeons feel there is less chance of developing kneecap pain using the hamstring graft versus the patellar tendon graft.
A new technique for grafting uses a portion of the quadriceps tendon, from the quadriceps muscles. This tissue has bone at one end and soft tissue at the other. This procedure combines some of the advantages of the patellar tendon reconstruction and the hamstring tendons reconstruction.

An orthopaedic surgeon will usually prefer to use a patient's own tissue for the graft. The patient's own tissue heals faster and more reliably than allograft tissue. In addition, allograft tissue has a risk of disease transmission, although this risk is extremely small.
For some patients, allograft tissue may be the better choice. Patients who have had numerous knee surgeries may not have sufficient tissue available for grafting. An allograft might be the best choice for an older patient who needs the least amount of invasion of the joint in order to heal without complications.
There are many types of devices used to secure the graft to the bone. Some examples are interference screws, screw/ washer, endobutton, and cross pins. Some are metallic and others are absorbed by the body over time. The type of graft procedure the surgeon chooses will determine the fixation technique.
ACL reconstructions are almost always done arthroscopically, although compound injuries may require open surgery. The repair is done with visualization by the arthroscope. One or two incisions are made to take the graft, drill tunnels in the bone, and to position it correctly.
ACL reconstruction can either be performed in an out-patient setting, or as an inpatient procedure with an overnight hospital stay.
 Non-operative Treatment
Non-operative Treatment
A good physical therapy program will focus on rehabilitation of the knee in two areas:
- Strength - The muscles surrounding the knee, particularly the hamstring muscles, must be strengthened. These muscles can then take on some of the ACL's job of stabilizing the knee joint.
- Proprioception - Proprioceptive nerves in the ligament send important information to the brain about where the body is in space. The brain then sends information to the muscles to tell them how to move the joint. The damaged nerves in the ligament must be retrained so that the muscles will move the joint properly.
A functional ACL brace will usually be prescribed to stabilize the knee and to prevent reinjury. Most functional braces incorporate a rigid frame. A trained specialist will fit the patient with the brace since a good fit is essential. Modern functional braces are lighter and much less bulky than older models. Patients find them easy to apply and comfortable to wear.
Operative Treatment
Following surgery, the patient will be started on a structured rehabilitation program. Patient commitment and involvement are essential for a good functional result. The specific exercises and program timelines vary depending on the graft source used, and whether surgical repair to other injured structures was performed.
The first phase of rehabilitation emphasizes range of motion, which is critical to avoid knee stiffness.
- A continuous passive motion (CPM) machine is used in the recovery room and the first night. This machine gently and steadily bends and straightens the patient's knee.
- Crutches are used for the first 7 -10 days after surgery for comfort. Full weight bearing would be painful.
- Riding a stationary bike without resistance and pool exercises to increase motion usually begin about 2 weeks after the surgery.
- Driving is allowed when the patient is comfortable and has mobility, often as early as 2 weeks after the operation.
The patient returns for an office visit about 2 weeks after the surgery so the incision and range of motion can be checked.
The second phase of rehabilitation incorporates strengthening and usually begins about 6 weeks after surgery.
- A sports cord (an elastic resistance strengthening tool) and the treadmill are initially used.
- Use of a stair-stepper or elliptical trainer is added at about 8 weeks.
- Strengthening using weights is allowed at 2 - 3 months.
The third phase of rehabilitation adds sport-specific exercises.
- Running is allowed at 3 months.
- Pivoting and twisting activities can begin at 4 to 5 months.
This phase is usually customized for the patient's sports and activity level.
The final phase of rehabilitation involves a supervised return to sports. This usually occurs approximately 6 months after reconstructive surgery.
 Are knee braces used after ACL reconstruction?
Are knee braces used after ACL reconstruction?
Bracing after an ACL reconstruction depends on the surgeon's preference. Some surgeons use no bracing while some use braces only during the rehabilitation phase. Still others recommend that patients always use a brace.
A post-operative brace is often used immediately after surgery. This is a large, sturdy brace that limits motion and helps protect the repair from an unexpected fall or twist. This type of brace is easily adjusted to accommodate the changes in the knee as swelling subsides.
A functional brace is lighter and less bulky and is often used during later stages of rehabilitation to protect the ACL reconstruction. Some surgeons recommend continued use of a custom-fit functional brace as a "safety-belt" during sports after this type of surgery.
What type of follow-up is done after an ACL reconstruction?
Usually, about a year following surgery, the doctor will evaluate the knee to measure the final results of the reconstruction in these areas:
- Motion
- Stability
- Symptoms such as pain or swelling
- How well the knee functions in daily living
- Whether or not the patient has been able to return to sports
Some of these follow-up exams have shown that 90 to 95% of patients with ACL reconstructions have good to excellent results.
What types of complications can occur with an ACL reconstruction?
Stiffness in the joint, or lack of extension, is the most common complaint. This is why it is important to wait for motion to return and swelling to go down before surgery, and to follow the rehabilitation instructions given by the doctor and therapist.
Failure of the graft, reinjury to the ACL, or injury to other structures in the knee are possible, and can cause recurrent instability. Blood clots and infection in the joint are very rare occurrences.
Can the ACL heal by itself?
Some knee ligaments, such as the medial collateral ligament (MCL), heal reliably without surgery. Some partially torn ACLs, particularly in children and adolescents, may also heal without surgery. However, a complete tear of the ACL rarely heals. This is probably due to the amount of energy involved in the injury, the lack of blood supply, and the interior location of the ACL. The torn ACL may scar back to the intact PCL within the knee, but this rarely returns stability to the knee. In fact, even when the ends of a torn ligament are sutured together (called a primary or direct repair), the ligament does not reliably heal. Therefore, surgery for a complete ACL tear (an ACL reconstruction) involves replacing the ACL with other tissue (a graft).
Is surgery always needed for an ACL tear?
Surgery is not required for all ACL injuries. Partial tears, in which a physical examination shows a relatively stable knee, may be treated with bracing and rehabilitation. Even some patients with complete ACL tears do not need reconstruction. These "copers" are typically older patients with lower physical activity, who do not participate in pivoting and cutting activities.
Why should the ACL be reconstructed?
One reason to reconstruct the ACL is to provide knee stability that allows for return to activities and sports. Another reason is to provide knee stability in order to prevent more injury, such as a meniscal tear, which may eventually lead to degenerative joint disease.
Is an MRI needed to diagnose an ACL tear?
An MRI is not always required to diagnose an ACL tear. An ACL tear can be accurately diagnosed with a physical examination. However, when the knee is very swollen and painful, an accurate examination can be difficult. Also, an MRI can be useful to reveal other associated injuries such as meniscal tears, a PCL tear, or injury to other supporting structures.
Which is the best graft to use for an ACL reconstruction?
There are advantages and disadvantages to the many technical aspects of an ACL reconstruction including the type of graft, methods of securing the graft, and rehabilitation protocols. There is no clear consensus as to which graft is best. In the end, the surgeon's experience with the chosen technique and the patient's commitment to the rehabilitation program are probably more important factors in a functional outcome.
When can I play sports again after ACL reconstruction?
Rehabilitation programs after ACL reconstruction are constantly evolving, shortening the return to sports. Most patients can start to return to their sports about 6 months after reconstruction.
Arnoczky SP: Anatomy of the anterior cruciate ligament. Clin Orthop 1983; 172: 19-25. Cannon WD Jr, Vittori JM: The incidence of healing of arthroscopic meniscal tears in anterior cruciate ligament-reconstructed versus stable knees. Am J Sports Med 1992; 20: 176-181.
Clancy WG, Ray JM, Zoltan DJ: Acute tears of the anterior cruciate ligament: Surgical versus conservative treatment. J Bone Joint Surg 1988; 70: 1483-1488.
Daniel DM, Stone ML, Sachs R: Instrumented measurement of anterior knee laxity in patients with acute anterior cruciate ligament destruction. Am J Sports Med 1985; 13: 401-407.
Daniel DM, Stone ML, Dobson BE, Fithian DC, Rossman DJ, Kaufman KR: Fate of the ACL-injured patient: A prospective outcome study. Am J Sports Med 1994; 22: 632-644.
Feagin JA, Curl WW: Isolated tears of the anterior cruciate ligament. 5-year follow-up study. Am J Sports Med 1976; 4: 95-100.
Fu FH, Harner CD, Johnson DL: Biomechanics of knee ligaments: Basic concepts and clinical application. J Bone Joint Surg 75: 1716-1725, 1993.
Johnson RJ, Beynnon BD, Nichols CE, Renstrom P: Current concepts review: The treatment of injuries of the anterior cruciate ligament. J Bone Joint Surg 1992; 74A: 140-151.
Noyes FR, Mooar PA, Matthews DS, Butler DL: The symptomatic anterior cruciate deficient knee. Part I: The long-term functional disability in athletically active individuals. J Bone Joint Surg 1983; 65A: 154-162.
Shelbourne KD, Nitz P: Accelerated rehabilitation after anterior cruciate ligament reconstruction. Am J Sports Med 1990; 18: 292-299.
Wojtys EM, Kothari SU, Huston LJ: Anterior cruciate ligament functional brace use in sports. Am J Sports Med 1996; 24: 539-546.
Montgomery KD, Elizabeth A. Arendt (ed). Anterior Cruciate Ligament Injuries, Orthopaedic Knowledge Update Sports Medicine 2. Illinois: American Academy of Orthopaedic Surgeons, 1999, 307 - 315










