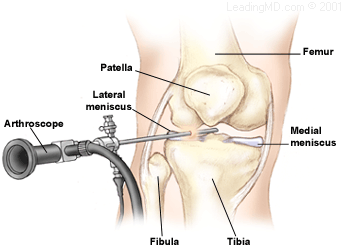
 How is a meniscus injury treated?
How is a meniscus injury treated?
When determining the treatment for a meniscal tear, the orthopaedic surgeon will consider the following factors:
-
The patient's activity level
-
The patient's age
-
The location of the tear and the type of tear
-
When the injury happened
-
Injury symptoms
-
Any other associated injuries
After considering these factors the doctor will choose to treat the injury non-operatively or surgically.
Non-operative Treatment
Many small meniscal tears will heal without surgical treatment. Also, some tears may have no symptoms and in other tears, symptoms may eventually disappear. Partial tears, degenerative tears, and stable tears may be observed for 2 - 3 months. If symptoms disappear, no surgery is needed. The use of a knee brace and restriction of activities may be recommended to prevent further injury.
Surgical Treatment
Surgical treatment for a meniscal tear may be indicated if:
-
symptoms are disabling or last for more than 2 - 3 months
-
a displaced tear causes the joint to lock
-
the anterior cruciate ligament is also injured - In this case, the knee is highly unstable and excessive motion exists within the joint. The meniscus is unlikely to heal without treatment.
-
the patient is a high-level athlete
If surgery is recommended, the procedure chosen is usually dependent on the location and type of meniscal tear. All procedures are performed through an arthroscope and usually don't require an overnight hospital stay.
Trephination/ Abrasion Technique
Partial Resection
Complete Resection
Meniscal Repair
Meniscal Replacement
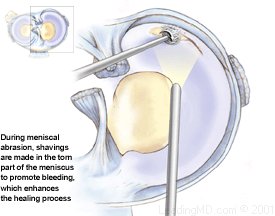
Trephination/ Abrasion Technique
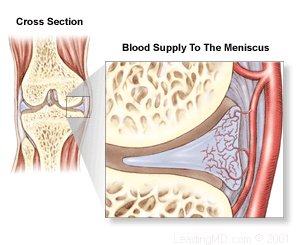
This procedure is used for stable tears located on the periphery near the meniscus and joint capsule junction, where there's a good blood supply. Multiple holes or shavings are made in the torn part of the meniscus to promote bleeding, which enhances the healing process.
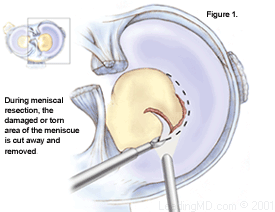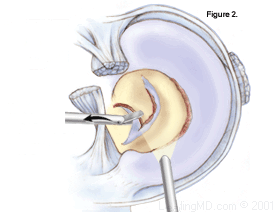
Partial Resection
This surgical procedure is used for tears located in the inner 2/3 of the meniscus where there is no blood supply. The goal is to stabilize the rim of the meniscus by removing as little of the inner meniscus as possible. Only the torn part of the meniscus is removed. If the meniscus remains mostly intact with only the inner portion removed, the patient usually does well and does not develop early arthritis.
Complete Resection
This procedure involves the complete removal of the damaged meniscus. This technique is only performed if absolutely necessary. Removal of the entire meniscus frequently leads to the development of arthritis.
Meniscal Repair
Repairs are performed on tears near the outer 1/3 of the meniscus where a good blood supply exists, or on large tears that would require a near-total resection. The torn portion of the meniscus is repaired by using either sutures or absorbable fixation devices. These devices include arrows, barbs, staples, or tacks that join the torn edges of the meniscus so they can heal.
Meniscal Replacement
Experimental attempts to replace damaged meniscus are seen as important recent advances in orthopaedic medicine. The new technology mentioned here has been performed at a few surgical centers across the country on a small number of patients.
-
Collagen meniscus implant - This is a scaffold of collagen inserted into the patient's knee. Over time, a new meniscus may grow within the joint. This procedure is currently in FDA trials in the United States and has just been approved as an accepted surgical procedure in Europe.
-
Meniscal transplant - This procedure involves transplanting a meniscus from a donor into the injured knee. Only a limited number of surgeons perform this procedure on a routine basis. The long-term outcomes are still being evaluated.



 How is a meniscus injury treated?
How is a meniscus injury treated?










