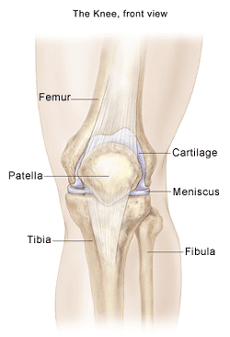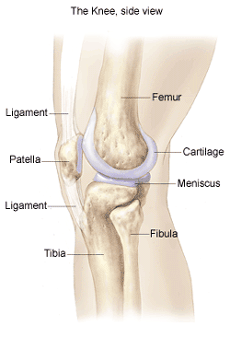
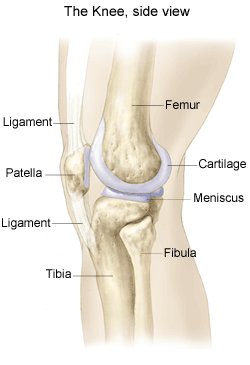
Patellofemoral pain syndrome (PFPS) is a common knee disorder, which often affects the senior athlete and those involved in running and jumping sports. Overuse, a change in activity, and an altered metabolic status are frequently responsible for the development of PFPS. Structural alignment and muscular weakness or imbalance may cause the patella (kneecap) to track improperly on the femur (thigh bone) during movement, leading to pain around the kneecap.
Other terms for patellofemoral pain are: retropatellar pain, peripatellar pain, anterior knee pain, and runner's knee.
Different disorders that cause pain around the kneecap include:
- infrapatellar tendonitis (jumper's knee), which affects the tendon just below the kneecap
- chondromalacia patella, which involves damage to the cartilage surface of the patella
- quadriceps tendonitis, which affects the tendon attachment above the patella
- plica syndrome, in which joint tissue becomes inflamed and/or stiff, causing pain and tightness in the joint
What is the patellofemoral joint?
As the knee bends and straightens, the patella slides within a slot on the femur called the trochlear groove. The patella moves in many directions within this groove to provide efficient, frictionless movement up and down, side-to-side, rotational, and tilting. The bone surfaces are covered with articular cartilage to make joint movement smooth.
What is patellofemoral pain syndrome and what can cause it?
Repeated abrasion on any of the surfaces of the patella and femur stresses the soft tissues of the patellofemoral joint and may even lead to a bone bruise. In some cases, the pain is caused by a weakening of the articular cartilage and/or swelling within the joint.
One or more of the following factors can lead to patellofemoral pain:
-
Overuse: the repetitive bending and straightening of the knee that occurs in running may lead to the disorder because of the increased pressure points between the patella and femur when the knee is bent. A constant bending motion, especially on the weighted leg, can irritate the patella and cause a bone bruise to form.
-
Alignment: The quadriceps alignment between the hip and the knee (the Q angle) is thought to affect patellar tracking. Patients with a larger than normal Q angle (greater than 20 degrees) may be more susceptible to patellofemoral pain because the patella has a tendency to track more laterally (to the outside). Pain may be felt more on the outside of the patella and femur because of increased pressure on these contact areas. The Q angle of growing female athletes enlarges as the pelvis widens during the maturing process, increasing the risk for patellofemoral pain.
-
Muscular weakness: A weakness or strength imbalance of the quadriceps muscles may alter the tracking of the patella.
-
Muscular tightness: Tight muscles and tendons may also affect patellar tracking. The muscular structures that cause movement in the knee and hip must be flexible. If any one muscle or muscle group is tighter than the rest, patellar instability can occur.
-
Flat feet (excessive foot pronation): Patients with little or no arch in the foot are also likely candidates for patellofemoral pain. As the foot rolls inward, the tibia compensates by rotating inward, disturbing the normal mechanics of the patellofemoral joint.
- A decrease in patellar mobility: the kneecap tightens, losing its normal ability to move in many directions